Eating Your Way to Clear Skin with Low Carb and FODMAP Diets
Is Your Gut Causing Your Breakouts? What You Need to Know About Low FODMAP Acne
Low FODMAP acne is a growing area of interest for people who have tried everything — cleansers, prescriptions, cutting out sugar — but still wake up to new breakouts. The idea is simple: certain carbohydrates in everyday foods (even “healthy” ones) are poorly absorbed in the gut, ferment in the intestine, and trigger inflammation that shows up on your skin.
Here’s a quick summary of how low FODMAP may help with acne:
- What it is: A diet that removes fermentable carbs (FODMAPs) to calm gut inflammation
- Who it may help: People with acne and digestive issues like bloating, IBS, or SIBO
- How it works: Fewer fermentable carbs → less gut fermentation → less systemic inflammation → calmer skin
- How long: Most people follow an elimination phase of 2–8 weeks before seeing changes
- Is it proven? Evidence is promising but still emerging — it’s better supported for rosacea than standard acne
The gut-skin connection is real, and the numbers back it up. In one survey, 75.3% of acne patients believed nutrition played a role in their skin — yet 87.4% said their dermatologist never discussed diet with them at all. That’s a huge gap between what patients suspect and what they’re being told.
For Ana — and millions of people like her — that gap is frustrating. You’re reading labels, eating your vegetables, and your skin is still breaking out. Sometimes, the culprit isn’t junk food. It’s the apple in your lunch bag or the garlic in your stir-fry.
That’s the FODMAP twist most people never see coming.
Understanding the Gut-Skin Axis: Why Low FODMAP Acne Treatment Works
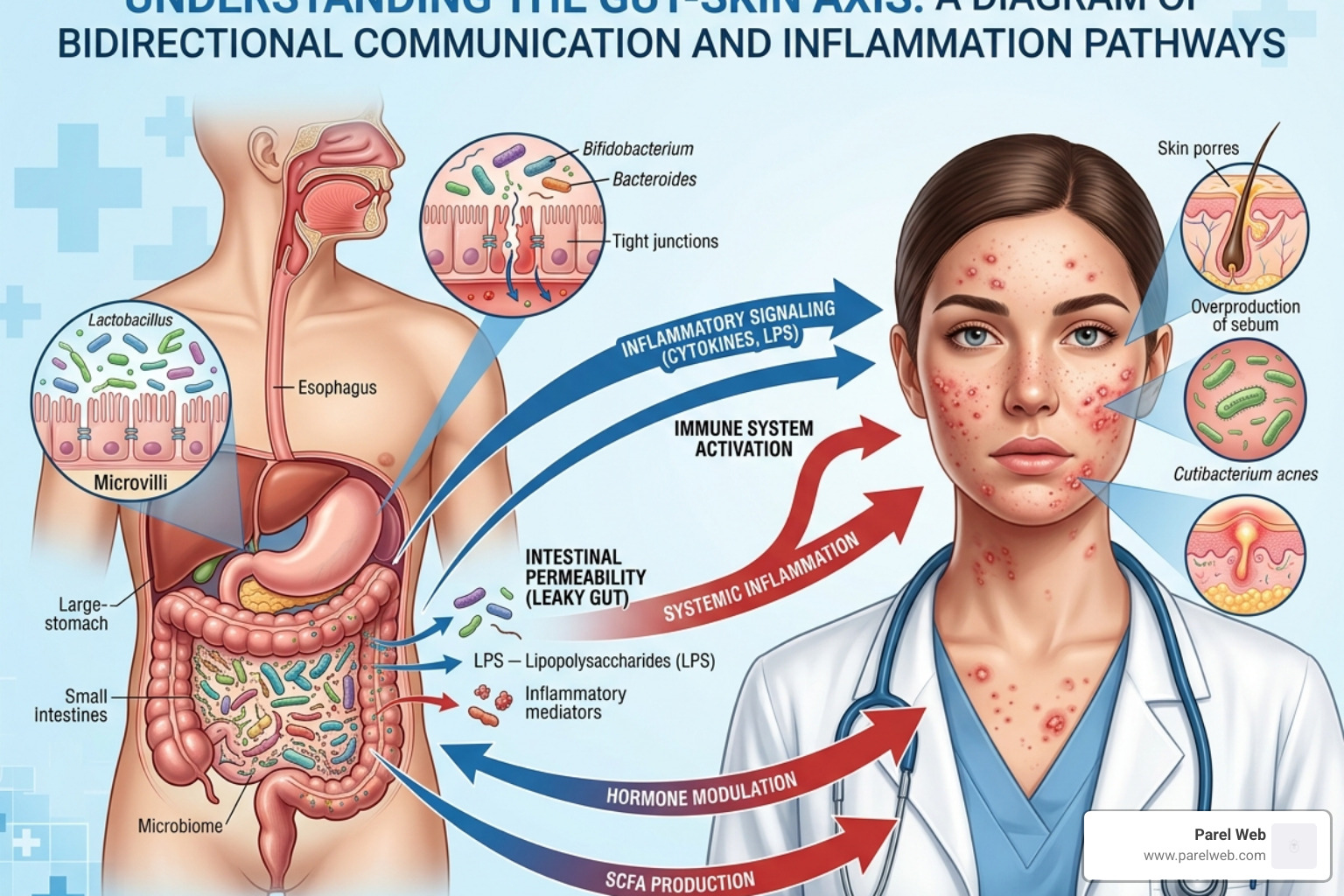
At Parel Web, we believe that beauty starts from within, specifically in the delicate ecosystem of your digestive tract. The “gut-skin axis” isn’t just a buzzword; it’s a biological highway. When our gut is unhappy, our skin is often the first to send up a flare-up.
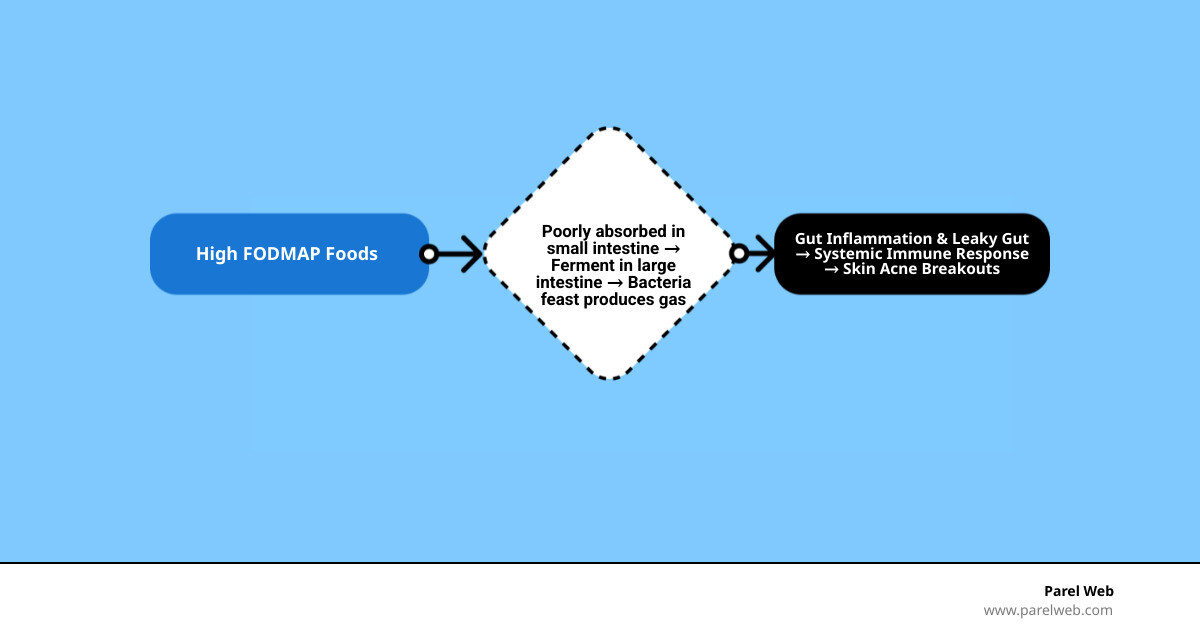
Approximately 70% of our immune system resides in the gut. When we consume foods that our body struggles to break down, it triggers an immune response. For those sensitive to FODMAPs (Fermentable Oligosaccharides, Disaccharides, Monosaccharides, and Polyols), these short-chain carbohydrates pass through the small intestine undigested and land in the large intestine. There, they become a feast for bacteria, leading to fermentation, gas, and “leaky gut” (intestinal hyper-permeability).
This process allows inflammatory compounds to escape into the bloodstream, eventually reaching the skin and triggering the production of sebum and proinflammatory cytokines. Research published in Linking diet to acne metabolomics, inflammation, and comedogenesis – PMC suggests that this systemic inflammation is a primary driver of modern acne.
The Role of SIBO and Rosacea
If you struggle with redness and flushing alongside your breakouts, you might be dealing with rosacea. Interestingly, the link between the gut and rosacea is even stronger than it is for standard acne. Studies have shown that patients with rosacea are ten times more likely to have Small Intestinal Bacterial Overgrowth (SIBO).
SIBO occurs when bacteria that should be in the large intestine migrate to the small intestine. These bacteria love to ferment FODMAPs. When we starve these bacteria through a low fodmap acne protocol, we often see a dramatic reduction in skin vascular reactivity. In one clinical review, treating SIBO with the antibiotic Rifaximin led to the complete resolution of rosacea symptoms in all 40 patients studied, with no relapses over three years. You can read more about these fascinating findings in Reexamining the Role of Diet in Dermatology.
Insulin, IGF-1, and Skin Flare-ups
While FODMAPs deal with fermentation, we can’t ignore the role of insulin. High-glycemic (hyperglycemic) carbohydrates cause a spike in insulin and Insulin-like Growth Factor 1 (IGF-1). This hormonal surge activates a signaling complex called mTORC1 and suppresses a protective protein called FoxO1.
The result? Your sebaceous glands go into overdrive, producing excess oil and promoting the “hyperkeratinization” (clogging) of pores. This is why many people find success combining a low FODMAP approach with a low-glycemic or low-carb lifestyle. For a deeper dive into how these dietary mediators affect your complexion, check out Evaluating the efficacy of dietary interventions on skin health: a comparative review of outcomes in acne and rosacea.
The Three Phases of the Low FODMAP Diet for Skin Health
Transitioning to a low fodmap acne diet isn’t a permanent “forever” restriction. We view it as a diagnostic journey to help you find your “Beleza saudável.” In April 2026, the gold standard for this protocol involves three distinct phases.
1. The Elimination Phase (2–8 Weeks)
In this phase, we swap out high FODMAP foods for low FODMAP alternatives. The goal is to “quiet” the gut and reduce systemic inflammation. This is the period where most people begin to see a reduction in new cystic acne and a calming of skin redness.
2. The Reintroduction Phase
This is where the detective work happens. One by one, we systematically reintroduce specific FODMAP groups (like fructose or lactose) to see which ones trigger a skin flare-up or digestive upset. You might find that you can handle honey (fructose) just fine, but a slice of wheat bread (fructans) results in a breakout the next morning.
3. The Personalization Phase
Once you’ve identified your triggers, you can return to a diverse, healthy diet that only excludes the specific foods that bother you. This ensures long-term gut health and skin clarity without unnecessary restriction.
For more details on using this method to pinpoint triggers, see Using The Low FODMAP Diet to Diagnose Hormonal Acne.
Identifying Your Personal Triggers
Keeping a food and symptom diary is essential. We recommend tracking not just what you eat, but how your skin looks and how your gut feels 12 to 24 hours later. Because FODMAPs cause issues through fermentation, the reaction isn’t always instant. You might eat a high-FODMAP meal on Monday night and see the “FODMAP acne” appear on Wednesday morning.
Common triggers to watch for include:
- Intestinal Permeability: Does dairy make you feel bloated and give you chin acne?
- Microbiome Diversity: Are you eating enough low-FODMAP fiber (like carrots and quinoa) to keep your “good” bacteria happy?
Long-term Sustainability and Risks
We want to be clear: a strictly low FODMAP diet should not be followed long-term without professional guidance. Many high-FODMAP foods, like onions and garlic, are excellent prebiotics that feed beneficial gut bacteria. Restricting them for years can lead to nutrient shortages (like fiber, iron, and calcium) and a decrease in microbiome diversity.
Our goal is always to find the least restrictive diet that keeps your skin clear. If you find you are reacting to almost everything, it’s time to work with a professional to address the root cause, such as SIBO or chronic stress.
High FODMAP Triggers vs. Skin-Safe Alternatives
It can be shocking to realize that “healthy” staples might be the reason for your low fodmap acne. Here is a quick reference table to help you make skin-safe swaps today.
| High FODMAP Trigger | Potential Skin Impact | Low FODMAP Skin-Safe Alternative |
|---|---|---|
| Garlic & Onions | High fermentation; SIBO trigger | Chives, green onion tops, or garlic-infused oil |
| Wheat / Rye | Gluten-related inflammation | Rice, quinoa, oats, or buckwheat |
| Apples / Pears | Excess fructose; feeds gut bacteria | Strawberries, blueberries, or oranges |
| Watermelon | High fructose and polyols | Cantaloupe or honeydew (in small amounts) |
| Milk / Soft Cheese | Lactose + IGF-1 (double hit) | Lactose-free milk, almond milk, or hard cheeses |
| Honey / Agave | Fructose spikes insulin | Maple syrup or stevia |
For a deeper explanation of why these “clean” fruits and vegetables can cause outbreaks, read FODMAPs: A Hidden Cause Of Acne In Seemingly Clean Fruits And Vegetables.
Low FODMAP vs. Low Glycemic and Keto Diets
While the low fodmap acne protocol focuses on fermentation, other diets focus on insulin.
- Low Glycemic (LG): Focuses on keeping blood sugar stable. Highly effective for reducing acne lesions.
- Ketogenic (Keto): A high-fat, very low-carb diet. While restrictive, it has potent anti-inflammatory effects that may benefit acne, though direct studies are still limited.
- Mediterranean Diet: Often considered the “gold standard” for overall health, emphasizing fish, olive oil, and vegetables. It is naturally lower in processed sugars and high in antioxidants.
In our experience, the best results often come from a “Low FODMAP Mediterranean” hybrid—focusing on anti-inflammatory fats and proteins while choosing low-fermentation carbohydrates. You can compare these strategies in Dietary intervention in acne management: review of the literature and future prospective.

Complementary Strategies for Clear Skin
Diet is a massive piece of the puzzle, but we love a holistic approach at Parel Web. To enhance your results, consider these additions:
- Probiotics: Specific strains like Lactobacillus can help modulate the gut-skin axis and reduce systemic inflammation.
- Zinc and Vitamin A: These are powerhouses for skin repair and sebum regulation.
- Hydration: Drinking 1.5L to 2L of water daily helps flush toxins and keeps skin plump.
- Stress Management: High cortisol can wreck your gut barrier, making you more sensitive to FODMAPs.
- Gentle Skincare: While you fix the inside, treat the outside with kindness. Look for ingredients like aloe vera, chamomile, and niacinamide to calm existing inflammation.
Frequently Asked Questions about Low FODMAP Acne
How long does it take to see results with a low fodmap acne protocol?
Most of our community members report a change in their digestion within days, but skin takes longer. Because the average skin cell turnover cycle is about 28 days, you should commit to the elimination phase for at least 4 to 8 weeks to see the full impact on your complexion.
Can a low fodmap acne diet help with hormonal breakouts?
Yes! Hormonal acne is often exacerbated by insulin spikes. By choosing low FODMAP, low-glycemic foods, you help stabilize your insulin levels. This, in turn, reduces the production of androgens and IGF-1, which are the main culprits behind those monthly jawline breakouts.
Is the low FODMAP diet safe for long-term acne management?
As mentioned, we don’t recommend a strict low FODMAP diet forever. It is a tool to identify triggers. Long-term, you should aim for a “personalized FODMAP” diet that includes as many prebiotic-rich foods as your skin and gut can tolerate.
Conclusion
The journey to clear skin isn’t always about what you put on your face—it’s often about what you put in your body. By understanding the link between low fodmap acne and your gut health, you take back control of your beauty.
We know it can feel overwhelming to navigate these dietary changes, but remember: you aren’t just “going on a diet.” You are learning the unique language of your own body. Whether it’s swapping your morning apple for a handful of strawberries or finally addressing that nagging bloat, every small step brings you closer to gut-skin harmony.
At Parel Web, we are here to support your transition to natural, healthy beauty. Embrace the process, listen to your gut, and let your inner health shine through your skin.

Ready to transform your routine? Start your journey to healthy beauty naturally with us today!